Choosing your treatment
Choosing your treatment
Depending on your type of prostate cancer (grade, stage, PSA rate), your age, your health status, your medical and family history, you may be able to choose your treatment from among several treatment options. It will then be important to have all the information on each option available to make an informed decision.
There are a number of treatments for prostate cancer available. Some treatments are standard (the currently used treatment), and some are still being tested in clinical trials.
Treatments currently used
- Active surveillance – Involves closely monitoring small, low-risk, slow-growing prostate cancer.
- Radical prostatectomy (open, laparoscopic, robotic) – Surgery that completely removes the prostate gland, as well as part of the urethra within the prostate and the seminal vesicles.
- Radiation therapy (external beam) – Radiation therapy uses radiation to shrink tumours and kill cancer cells.
- Brachytherapy – Brachytherapy irradiates the prostate from an internal source to shrink tumours and kill cancer cells.
- Hormone therapy – Hormone therapy deprives cancer cells of the male hormones (e.g., testosterone) they need in order to grow.
- Chemotherapy – Drugs that treat aggressive cancer. These drugs affect both cancer cells and healthy cells. Healthy cells tend to regenerate whereas cancer cells struggle to do so.
There are also several approaches and strategies for preventing or treating bone metastases, treat them or to relieve symptoms and bone pain.
Note
Focal therapy – Other options such as cryotherapy and IFHU/HIFU are currently under study. It should be noted that these are not standard treatments. They are used when the cancer is believed to be still limited to the prostate. However, neither of these techniques can currently be considered a viable alternative to standard prostate cancer treatment options. And since their long-term effectiveness is not known, few healthcare centers offer them in Canada.
Clinical trials
One way to access new treatments before they become widely available is to participate in clinical trials. A clinical trial is a research study that uses volunteers, called participants, to test new ways of preventing, detecting, treating, or managing prostate cancer or other illnesses. Some clinical trials help determine whether or not a new drug or device is effective and safe.
Participating in a clinical trial is a valuable contribution to research as clinical trials answer important questions that can lead to better health outcomes. Participation can be a good way for participants to access free and new treatments and to be closely monitored by healthcare workers. To learn more about clinical trials, speak with your healthcare team.
Finding a clinical trial can be a difficult and tedious process. To address this issue, our partner Q-CROC developed Onco+, a free support service available to anyone looking for an oncology clinical trial in Quebec.
If you would like to learn more about oncology clinical trials in Quebec and consider whether participating in a clinical trial might be an option for you, please visit the website of our partner Q-CROC.
Additional clinical trial site:
- Canadian Cancer Trials: Canadian Urological Association
Alternative medicine
Complementary and alternative treatments include a wide range of approaches and therapies. It is important to understand the differences between conventional medicine, complementary therapies, and alternative therapies.
- Traditional medicine – Medical or surgical treatments that are accepted and practiced within the Canadian healthcare system. The best available research has shown these treatments to be effective and safe. Radiation therapy is an example of conventional medicine.
- Complementary therapies – Therapies used with or alongside conventional medicine, often to help people cope with cancer, treatment, or side effects. More research is needed to find out if they are safe and effective. An example of a complementary therapy is using meditation to help with stress or anxiety during treatment.
- Alternative therapies – Therapies used instead of conventional medicine. Alternative therapies have not been scientifically proven to be safe and effective. Following a special diet to treat prostate cancer instead of conventional treatments is an example of alternative therapy. Delaying or refusing conventional therapies in preference of using alternative therapies can have serious health consequences.
Discuss all treatment decisions with your healthcare team.
The diagnosis of prostate cancer greatly influences the choice of treatment. In fact, the results of the biopsy and the various tests determine two key indicators, namely the grade (Gleason score) and the stage of prostate cancer. The grade specifies the degree of aggressiveness of cancer while the stage indicates its degree of spread. These two indicators make it possible to determine the level of evolution of prostate cancer: localized, locally advanced, or metastatic. Our diagnostic page deals in detail with the type and risk of progression.
Risk of progression of prostate cancer
Prostate cancer can also be classified according to the risk of progression or recurrence – low risk, intermediate risk, or high risk of progression. For this evaluation, which may influence the therapeutic approach, consideration is given to the clinical stage, PSA, and Gleason score.
For example, your doctor may suggest a more aggressive treatment if your risk of recurrence is high. On the other hand, if your risk of progression is low, you could be offered active surveillance without receiving immediate treatment.
Localized prostate cancer
Localized prostate cancer is contained within the prostate, in other words, it has not spread outside of the prostate. Many localized cancers are often not very aggressive and tend to grow slowly. Because of this, chances are high that this type of cancer will not cause you any problems in your lifetime. However, some localized cancers grow more quickly than others and can spread to other parts of your body. There is no perfect treatment for localized cancer; each treatment has its strengths and weaknesses. Discuss the possible courses of treatment with your urologist.
Locally advanced prostate cancer
Locally advanced prostate cancer is cancer that has begun to break out of the prostate, but not too far. It may have spread beyond the boundaries of the prostate (capsule) into the neighboring regions of the seminal vesicles, pelvic nodes, bladder, rectum, or pelvic lining. Selecting the best treatment depends on the extent of its spread.
Metastatic prostate cancer
Metastatic prostate cancer is cancer that has spread to other parts of your body — far from your prostate. Metastases originating from the prostate most often develop in the bones and lymph nodes. Bone pain, fatigue, and weight loss are all symptoms associated with advanced cancer. Advanced prostate cancer cannot be cured. There are, however, many treatments that can help reduce symptoms and keep your cancer under control for several years.
In recent years, several treatments initially used after the failure of hormone injection, such as chemotherapy and/or next-generation hormone therapy in the form of tablets, are now sometimes used when a new diagnosis of metastatic prostate cancer is made.
What 2023 research says
In patients with prostate cancer that has spread significantly throughout the body, treatment options beyond just hormone injections, such as triple therapy (standard hormone therapy, chemotherapy and oral tablets), should be discussed with your doctor.
As such, here is a video clip that might interest you with Dr. Aly-Khan Lalani, Medical Oncologist at the Juravinski Cancer Centre and Assistant Professor at McMaster University, in Ontario, Canada, following the ASCO-GU scientific conference in 2023.
Other types of prostate cancer
Recurrence
The recurrence of cancer can happen when some cancer cells survive after your initial treatment. Cancer can recur in the same place or it can be detected in another part of your body. The latter is also known as a metastatic recurrence. The next treatment step depends on the location of the recurrence.
Castrate resistant prostate cancer (CRPC)
Hormone therapy can keep the spread of cancer under control for a number of years. However, with time, cancer may become castrate-resistant and start to grow again. That is to say, cancer is able to replicate despite castration (the low level of testosterone). The following terms were also used in the past in reference to castrate-resistant prostate cancer (CRPC): hormone-resistant prostate cancer, androgen-independent prostate cancer, and hormone-refractory prostate cancer.
Treatments exist to cure this type of cancer but differ depending on whether metastases are present or not: new generation hormone therapy – apalutamide (Erleada), enzalutamide (Xtandi) and abiraterone acetate (Zytiga) – is part of the combination treatments to treat this type of cancer.
What the research says in 2023
The addition of a targeted therapy like PARPi, a new approach in the therapeutic arsenal, the fruit of intensive research in recent years, should be discussed with your doctor, given their results on the progression of the cancer and on the potential improvement in the lifespan of the patients. It goes without saying that scientists are still trying to determine which patients are best suited to these types of combinations.
As such, here is a video clip that might interest you with Dr. Aly-Khan Lalani, Medical Oncologist at the Juravinski Cancer Centre and Assistant Professor at McMaster University, in Ontario, Canada, following the ASCO-GU scientific conference in 2023.
Who will care for you?
Once prostate cancer has been diagnosed, it is usually urologists and radiation oncologists who treat your cancer. If metastases are present, especially when using chemotherapy, a medical oncologist will often consult other health professionals.
Your healthcare team—consisting of your family doctor, radiation oncologist technicians, and volunteers—is there for support and comfort.
Factors to consider
Prostate cancer is a complex disease. Many personal or cancer-related factors may influence the choice of treatment in a given patient. It is important that you learn as much as you can about your cancer and the treatment options available to you, including potential side effects. This will allow you to have an informed discussion with your doctor and establish a treatment plan that is right for you. Decisions about your treatment are normally based on:
- Your type of prostate cancer
- Your PSA rate
- Your stage and grade (Gleason score)
- Your age and your life expectancy
- Your general state of health
- Your personal preference for treatment
Keep in mind that a positive diagnosis does not mean that you will be automatically treated and that an early detected cancer can be curable, if not controllable in the long term.
Choosing treatment can be difficult
Be sure to take the time to think about what is good for you and to get all the information you need. You will have an informed discussion with your doctor and choose the treatment option that is right for you.
You should also be aware that research is now providing increasingly precise treatments that target specific forms of cancer. In addition, treatment protocols now include many strategies to treat advanced disease. Click here to learn more about your treatment options based on your type of cancer.
Talk to your doctor
Men recently diagnosed with prostate cancer experience significant psychological distress filled with anxiety and fear, which can make it difficult to process information. This makes it very difficult to make an informed decision, especially when it could be one of the most important decisions of your life. This is why your doctor-patient relationship is crucial. Your doctor-patient relationship should be based on open communication and trust. Your doctor should see you as a human being with psychological, psychosocial, emotional, and cultural needs. You need to work as a team with your doctor to treat your prostate cancer most effectively.
Suggestions
Here are a few points to make your doctor’s visit as efficient as possible:
- Don’t be afraid to ask questions about your disease, treatments, and side effects.
- Keep a running list of your questions as they come to mind.
- Take a relative or friend with you.
- Taking a second appointment may be a good option for thinking and compiling questions.
If your doctor is giving you too much information at one time, let him or her know. There is nothing wrong with letting your doctor know how much information you can absorb in a single visit.
The right doctor for me
It is very likely that you will meet many people who are good resources and can help you. However, once you have been diagnosed with prostate cancer, your primary doctor will be your urologist. Your family doctor will also be informed of your diagnosis in order to monitor your overall health. Your urologist is probably the one you will speak to most. If necessary, you may be referred to a radiation oncologist, medical oncologist, or doctor specializing in palliative care.
How to know if your specialist is the right one for you?
By clicking here , you will find several questions you can ask if you are awaiting a diagnosis or if you have received a diagnosis of prostate cancer.
Help manage your treatment
You can participate in managing your care by keeping a personal medical record of your health status and ensuring that all your doctors receive a copy of your test results.
During each medical visit, you can inform your doctor about visits to other specialists. This approach will facilitate communication among each healthcare professional responsible for your care.
Seek a second opinion
It is important that you have enough information to really understand your situation. This will help you feel more in control of your life and help you make decisions.
If, for whatever reason, you are not comfortable with your doctor, ask for a second opinion. Doing so does not mean you are questioning your doctor’s competency. Certain elements of the doctor/patient relationship may encourage you to consult another specialist.
In addition, each doctor may have a different way of approaching the situation. It is important to develop a relationship of trust with your urologist.
Ask yourself the following questions:
- Does my doctor spend enough time with me?
- Are all my questions being answered?
- Is the language my doctor is using clear or is it too technical or medical?
- Is there a language barrier?
- Is my doctor’s office too far away from my home?
Perhaps you and your family need more reassurance about the possible treatment options and what would be the best approach to treat your cancer.
Seeking a second opinion is perfectly acceptable if you feel the need. Just let your urologist know—they may be able to suggest someone or give you information on how to get a copy of your chart.
Additional Information - Treatment options

How I coped with prostate cancer
A man with prostate cancer shares the challenges of his cancer experience.

Urologist’s advice: Treatments and information on prostate cancer
Learn more about the role of the urologist and the importance for a patient to gather adequate information after receiving a prostate cancer diagnosis.

Diagnosis and treatment
Recently diagnosed with cancer? Educate yourself to fully understand your situation.
Your role as a patient
You’ve been diagnosed with prostate cancer? Your role is as important as that of your medical team.
Biopsy: Understanding your report
This webinar clarifies biopsy reports, pathologists’ roles, and how results confirm or rule out prostate cancer.

Prostate cancer: Tests, imaging and biomarkers
This webinar covers various tests and exams for diagnosing and monitoring prostate cancer.

Prostate cancer prognosis and survival
After a prostate cancer diagnosis, questions about survival, cure rates, and quality of life can arise.

Tailored prostate cancer treatment
Over the years, prostate cancer treatment has immensely progressed. Doctors can now provide patients with a more tailored treatment. Indeed, advances in science, technology and surgical techniques have enabled medical teams to offer more personalized prostate cancer treatments.

How is prostate cancer staged?
The grade and stage of prostate cancer help determine the evolution of the disease. The grade refers to the degree of aggressiveness of the prostate cancer and can be assessed through the Gleason score. Cancer stage, meanwhile, refers to the degree of spread of cancer cells.. This article will cover the concept of prostate cancer […]

Prostate cancer: Screening or no screening
Prostate Cancer can be cured quite easily, but you still have to take an early screening to be on the safe side.
Sources and references
Last medical and editorial review: April 2024. See our web page validation committee and our collaborators by clicking here.
Relevant and additional information
Here, you’ll find a selection of key pages and resources that may address your questions or concerns. Scroll through to explore essential information available on our site.

Do you have a curved penis?

Can I prevent BRCA-related prostate cancer?

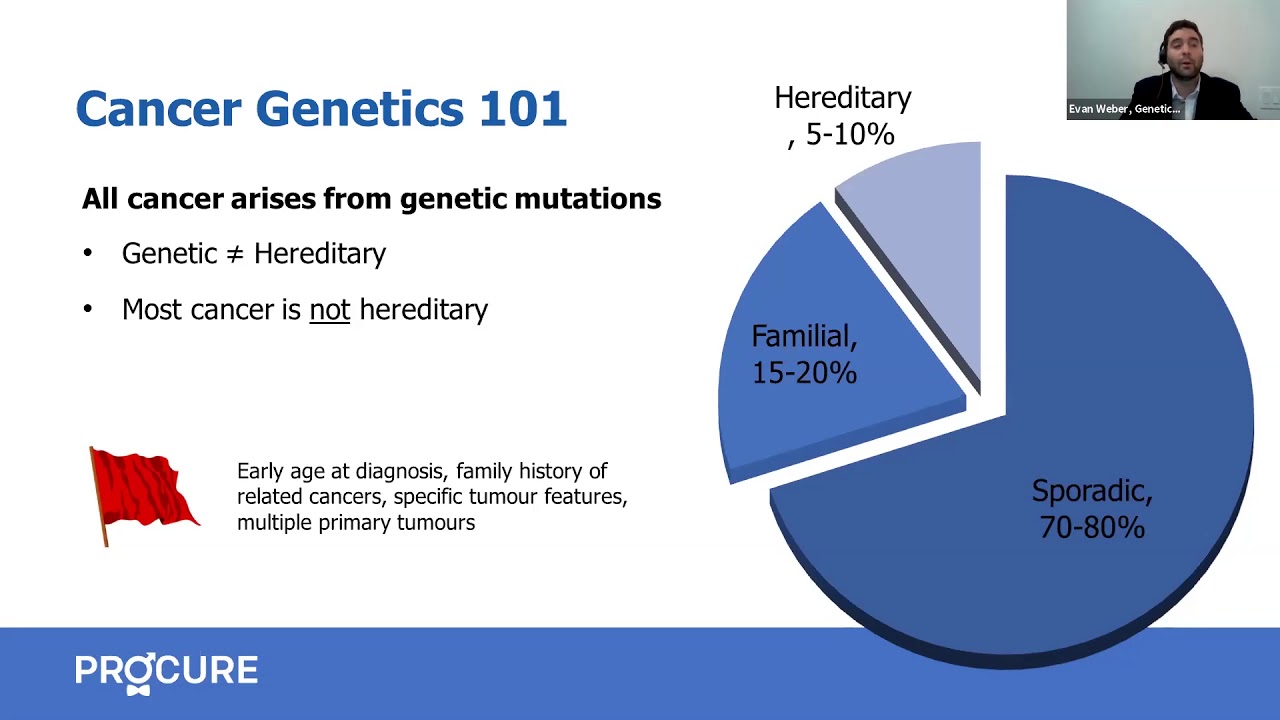
Is prostate cancer hereditary?
Genetics and prostate cancer

Symptoms, risk and screening

From prostate to screening