Women of Courage
- Testimonials
- Women of Courage
- Testimonials from women
- For additional inspiration
Women of Courage
Here are testimonials written by women acting as caregivers for men affected by prostate cancer. You can send us your testimonial by writing to info@procure.ca.
Testimonials from women

Here’s my testimony as a woman, I hope it will encourage others.
We learned in October that my husband (58 years old) had a grade 7 cancer despite a PSA of 3.2. His doctor at Maisonneuve-Rosemont was super conscientious; given that my husband had the hereditary factor and his PSA was unstable, he didn’t take any chances and had him undergo a biopsy which turned out to be positive. We had no idea what was going to happen; for us, it was the unknown… Discover the rest by clicking here


In 1994, my father learned that he had prostate cancer. He was 65 years old, and I was 29. When I was told the news, I was overcome with anxiety. It seemed unbelievable to me. Just thinking about it scared me. At first, I didn’t really seek information about the disease, as if I feared admitting the truth. Nevertheless, from that moment on, prostate cancer diagnoses seemed to come from everywhere: my uncle (my father’s younger brother) also learned that he had the disease, and shortly after, I discovered that my new friend’s father had just undergone a radical prostatectomy… Discover the rest by clicking here

“It’s cancer, Ben, my husband, had said on my office voicemail. I’ll probably need surgery. The risk of temporary incontinence is 95%, and the risk of erectile dysfunction can be high, depending on the type of procedure. By having the surgery, I have an 85% chance of being cured.” My husband believed in honesty, but this time, he had outdone himself. Even though I’ve worked in the healthcare field for many years, nothing in my career had prepared me for the emotions that overwhelmed me… Discover the rest by clicking here

In recent years, I’ve embarked on a journey with my husband that has been both enlightening and educational. Together, we’ve navigated the various steps to take with specialists regarding his illness. They all arrived at the same conclusion: prevention.
Prevention is becoming increasingly important because it saves and prolongs lives. That’s what we’ve learned. We’ve also learned that together, we can do even more. We must lend a hand, share knowledge, and help others benefit from it to build a stronger, more educated community about the disease. We’re all part of the same community, the community of humankind, so let’s help each other strengthen and extend our lives together.
Wishing everyone a good life.
Read the testimonials written by men on prostate cancer.
Video testimonials
On our YouTube channel, you can watch testimonials told with kindness and candor by individuals affected by prostate cancer. We are very grateful to them. You can watch them by clicking here.
If you wish to do the same, don’t hesitate to contact us at info@procure.ca so we can guide you on producing your own video testimonial and how to send it to us.
Are you looking to make a difference?
Prostate cancer and the development of research tools to fight this cancer are causes close to your heart? Become a volunteer for PROCURE! With your help, we can increase our outreach to the public and raise awareness about this disease. To learn more, click here.
Other pages that might interest you
Additional Information - Testimonials

How I coped with prostate cancer
A man with prostate cancer shares the challenges of his cancer experience.

Urologist’s advice: Treatments and information on prostate cancer
Learn more about the role of the urologist and the importance for a patient to gather adequate information after receiving a prostate cancer diagnosis.

Diagnosis and treatment
Recently diagnosed with cancer? Educate yourself to fully understand your situation.
Your role as a patient
You’ve been diagnosed with prostate cancer? Your role is as important as that of your medical team.
Active surveillance as a treatment option?
Did you know that in many cases it is not necessary to treat prostate cancer?

Surveillance, surgery or radiation therapy?
Diagnosed with prostate cancer? Several treatment options are available based on the stage, age, and your health.

Urinary and sexual problems after treatment
Prostate cancer treatments can lead to side effects, such as erectile dysfunction and urinary incontinence, which vary in intensity and duration.

What happens after my diagnosis of prostate cancer ?
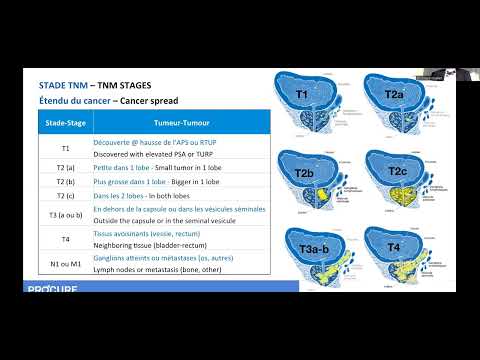
The diagnosis of prostate cancer greatly influences the choice of treatment. Indeed, the results of the biopsy and the different tests and scans measure two key indicators: the grade and stage of prostate cancer. The grade determines the degree of aggressiveness of the cancer while the stage indicates the degree of spread. Both indicators are […]

What are the prostate cancer treatment options?
There are several treatment options available for patients suffering from prostate cancer. The doctor adapts the treatment plans to meet the unique needs of each person and determines which option will lead to the most optimal results. Treatment should therefore take account of the progress of the disease, health status, age, opinions, preferences and expectations […]
What are my treatment options?
Under 70 years old Men in their fifties or sixties are more likely to die from prostate cancer than older men because the disease has more time to evolve or reappear. It is therefore very important to treat the cancer as soon as possible. In general, when the prostate cancer is localized, the most effective […]
Sources and references
Last medical and editorial review: April 2024. See our web page validation committee and our collaborators by clicking here.


