Enlarged prostate
On this page:
Discover our animated video!
Symptoms, risk and screening
Are you over 50 years old, or have you been having urinary problems for some time now? This video is for you! Several diseases can affect your prostate, and it’s important to detect them early. Let’s take a closer look.
Overview
Benign prostatic hyperplasia (BPH)
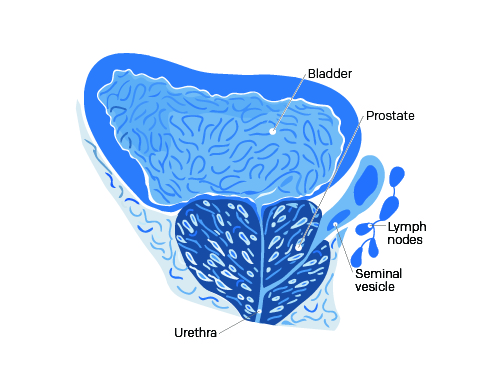
Benign prostatic hypertrophy (BPH) or enlarged prostate is characterized by an increase in the volume of your prostate due to an excessive multiplication of your cells. It is a natural part of getting older. This increase or growth can compress your urinary canal (the urethra), causing some urinary symptoms.
From the age of 50, it affects almost all men as they get older and about 25% of them will need to be treated.
Benign prostatic hyperplasia is not a form of prostate cancer and does not increase the risk of developing prostate cancer.
The exact cause of BPH remains unknown, although links may be established with the high-fat diet, family history, sedentary lifestyle and hormones.
Not all men with BPH experience symptoms, but if the prostate enlargement presses on the urethra (the tube that carries urine from the bladder out of the body), it could result in the following symptoms.
Symptoms
 In the early stages of BPH, there are no signs and symptoms. These appear when the prostate puts pressure on the urethra and bladder and cause changes in urination.
In the early stages of BPH, there are no signs and symptoms. These appear when the prostate puts pressure on the urethra and bladder and cause changes in urination.
The most common signs and symptoms
- More frequent urination (urinary frequency), especially at night
- A strong or sudden urge to urinate (urinary urgency)
- Difficulty starting or stopping the urine stream (called straining)
- Weak or slow urine stream
- Interrupted urine flow
- Being unable to empty the bladder completely
- Difficulty controlling the bladder (leaks)
- Pain or a burning sensation during urination
- Difficult or painful ejaculation
- Blood in the urine or semen (rare)
Risks and complications
- Urinary tract infection
- Urinary calculus
- Acute urine retention (emergency)
- Chronic urine retention
- Renal insufficiency if not cared for
Diagnosis
If you have unusual symptoms of BPH or if your doctor thinks you might have BPH, you will be sent for tests. They could include the following:
Medical history and physical examination
- A digital rectal exam (DRE) to ascertain the size of the prostate
- A questionnaire to assess the severity of the bladder disorder and how they affect the man’s quality of life
Urine Tests
- Urine analysis
- Urinary flow measurement (urodebitometry)
- Keeping a urination journal over several 24-hour periods
Blood tests
- Prostatic antigen specific (PSA)
- Blood urea nitrogen
- Creatinine
Imaging
- Ultrasound of the kidneys, bladder and prostate
- Ultrasound to determine how much urine remains in the bladder after urination (residual urine)
These tests and examinations are used to confirm a BPH diagnosis, to rule out other problems such as urinary tract infection or prostate cancer, and to check for any BPH-related complications.
Treatments
 Medicated (or not)
Medicated (or not)
Watchful waiting & lifestyle changes
Watchful waiting consists in carefully observing the person without administering any treatment, since a certain proportion of men may see a spontaneous improvement in symptoms. Changes in lifestyle habits include avoiding certain foods (coffee, tea, alcohol), decreasing the amount of fluids ingested before bedtime, moderating daily fluid intake (1.5-2.0L / day), and avoiding constipation.
5-alpha-reductase inhibitors
These drugs block the transformation of testosterone into dihydrotestosterone in the prostate. Dihydrotestosterone appears to be the cause for enlargement of the prostate. They take several months to reduce the size of the prostate and relieve symptoms. These medications can prevent secondary BPH complications (acute urinary retention, bleeding, etc.). By reducing the size of the prostate, they also decrease the level of PSA that will need to be closely followed. The two drugs in this category are:
Side effects may include:
- decreased sexual desire
- erectile dysfunction
- reduced amount of semen in ejaculation
- breast swelling or tenderness
Alpha-blockers
They are drugs that relax the muscles around the prostate to reduce pressure on the urethra and decrease symptoms affecting urine flow. They have a quick effect (24-72 hours) on urinary symptoms. The most common alpha-blockers used for BPH are:
Side effects may include:
- dizziness
- fatigue
- headache
- low blood pressure
Surgery
Surgery may be used to treat BPH in cases where the symptoms are severe severe, if the man is totally unable to urinate, when drug therapy has been ineffective, or if the man does not want to take daily medication.
Transurethral resection of the prostate (TURP)
TURP removes prostate tissue in order to reduce the size of the prostate. It is the surgery most commonly used to treat BPH. This is the most common surgical procedure for BPH.
- It is performed under general or spinal anesthesia.
- A special tube with light and a camera (resectoscope) is inserted into the urethra into the prostate.
- The surgeon can observe the inside of the urethra, prostate and bladder.
- The excess tissue of the prostate is removed in the region that surrounds the urethra. The excision can be done using a variety of techniques (electric, laser, etc.)
- A catheter is placed in the bladder to allow the urine to flow.
- The catheter is removed as soon as there is no more blood in the urine (usually after 24 hours).
Side effects of TURP may include:
- bleeding
- infection
- retrograde ejaculation
- new or minimally improved irritative urinary symptoms (frequent urination, urgency, etc.)
- erectile dysfunction – rare
- incontinence – rare
Some men may have to undergo a second intervention (10% of men after 10 years). Other surgical or radiological techniques performed under local anesthesia may be performed, but their long-term effectiveness remains to be determined.
We are here for you
You have questions or concerns? Don’t hesitate. Contact us at 1-855-899-2873 to discuss with one of our nurses specialized in uro-oncology. They are there to listen, support and answer your questions, and those of your family or your loved ones. It’s simple and free, like all of our other services.
Also take the time to visit each of our pages on this website, as well as our YouTube channel, in order to get familiar with the disease, our expert lectures, our section on available resources, the support that is offered to you, our events and ways to get involved to advance the cause.
Staying Informed
Pages that might interest you
Want to know more? Just click on one of the links below.
The latest PROCURE news that might interest
Every week we publish a blog article. Here’s some we chose for you.
The medical content and editorial team at PROCURE
Our team is composed of urologists, and nurses certified in uro-oncology with a deep knowledge of prostate cancer and other diseases related to the genitourinary system. Meet our staff by clicking here.
Sources and references
- Prostate Cancer – Understand the disease and its treatments; Fred Saad, MD, FRCSC and Michael McCormack, MD, FRCSC, 4th et 5th editions
- Canadian Cancer Society
- Prostate Cancer Foundation-PCF.org
- National Cancer Institute-USA
- American Cancer Society
- Memorial Sloan Kettering Cancer Center
- Prostate Cancer UK
Last medical and editorial review: September 2023
Written by PROCURE. © All rights reserved




