Radical surgery
Overview
Surgery is a common treatment for prostate cancer. Surgery is used to potentially cure the cancer by completely removing the tumour or to reduce urinary symptoms.
The type of surgery done depends mainly on the stage of the cancer and other factors, such as your age, general health, and life expectancy. Side effects of surgery depend on the type of surgical procedure.
Types of surgery
Radical prostatectomy
Radical prostatectomy is the most common surgical procedure for treating localized, low-risk, intermediate-risk or high-risk prostate cancer. It is a major surgery offered to men in good health.
A radical prostatectomy is the total removal of your prostate and the surrounding tissues. It is done as a potential cure for prostate cancer as it removes all cancerous cells. It can be combined with other treatments—for example, surgery followed by radiation therapy if needed.
Pelvic lymph node dissection
Sometimes prostate cancer with only microscopic spread to your lymph nodes can be cured with surgery. How do you know if your cancer has spread to your nodes? Thanks to modern investigative techniques, it is rare that we have to wait until the operation to realize that the cancer is too widespread to be able to perform a prostatectomy.
That being said, if your cancer is more aggressive and you choose to go with radical surgery, your surgeon will remove your major pelvic lymph node groups during the operation. It is not necessary to remove them if your cancer is at a low risk of progression.
Transurethral resection of the prostate
Unlike radical prostatectomies where your prostate and its capsule are removed, a transurethral resection of your prostate (TURP) consists of removing the internal lining of your prostate through your urethra while leaving your prostate capsule in place. This is the most common surgical procedure for benign prostatic hyperplasia (BPH or enlarged prostate).
In general, transurethral resection of the prostate (TURP) is usually given to relieve urinary problems caused by a prostate that has increased in size and is compressing the urethra. It is also used as a palliative treatment to relieve urinary obstructions in patients with advanced prostate cancer who are not healthy enough to undergo radical surgery.
Is it for you
You may opt for this surgery:
- if you have early stage cancer that has not spread outside the prostate (stage 1 or 2)
- if your cancer has spread locally outside the prostate (stage 3)
- if you have a life expectancy of at least 10 years
- if you are less than 75 years of age, will depend on the individual
- if you are healthy enough to undergo anesthesia and surgery
Reasons for choosing surgery
A radical prostatectomy is effective in the early stages of cancer when it is still confined to your prostate. Chances for recovery are excellent and it offers a high probability for long-term survival (more than ten years).
- However, it is also the most aggressive of treatments and therefore has the greatest risk of side effects. Radical prostatectomy is a major surgery.
- The younger and healthier you are, the more successful your recovery is likely to be. When thinking about surgery, you must consider the effect it will have on your life and weigh the possible benefits against the possible risks.
Surgical techniques
 Techniques to surgically remove the prostate include open surgery, hand-assisted laparoscopic surgery and robot-assisted laparoscopic surgery.
Techniques to surgically remove the prostate include open surgery, hand-assisted laparoscopic surgery and robot-assisted laparoscopic surgery.
Open surgery
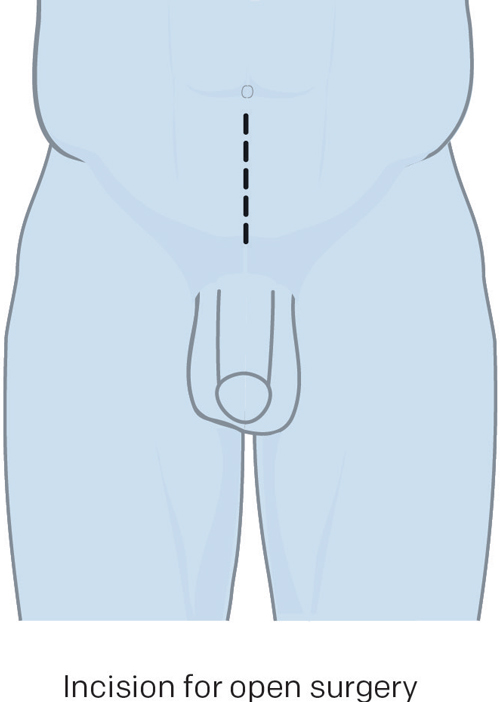
Traditionally, surgeons perform open radical prostatectomies through an incision in the lower abdomen (hence the term “open surgery”). This surgery allows for the removal of your pelvic lymph nodes before your prostate is removed.
Experienced surgeons are able to identify your erectile nerves and separate them from either side of your prostate in order to spare them from damage during the operation.
- This nerve-sparing technique reduces the risk of sexual dysfunction by 50%.
- It can be employed if the size and location of the tumour allow for it: if your tumour is too large or aggressive, the surgeon will not be able to save your nerves.
Advantages of this technique
This operation is available in most hospital centres in Quebec and across Canada.
Disadvantages of this technique
This nerve-sparing technique is not used by all surgeons since it is more complicated and delicate than the traditional method. You should speak to your doctor about the procedure to be used.
Hand-assisted laparoscopic surgery
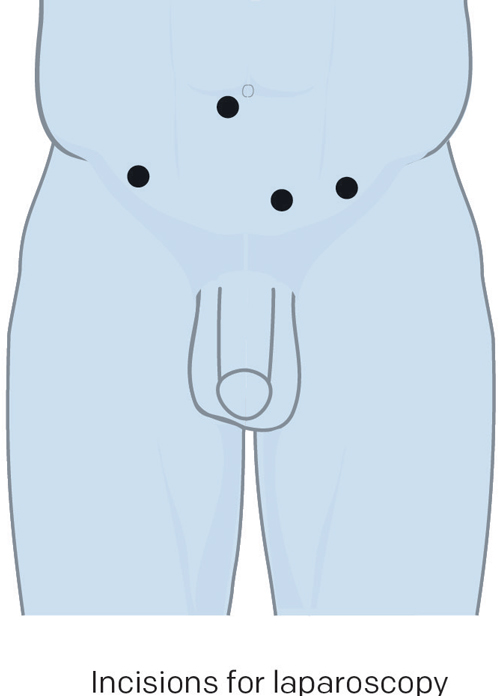
Instead of a single incision, five or six small ones (about one centimetre in length) are made in the lower abdomen. Long, slim surgical instruments are inserted through these incisions to guide the operation.
A telescopic instrument called a laparoscope is inserted into the abdomen through a small incision at the belly button.
A camera attached to the laparoscope allows surgeons to see inside the abdomen and perform the surgery without having to make a large incision.
Advantages of this technique
While this technique generally shortens recovery time, it is not proven to be any more effective than open surgery performed by an experienced surgeon.
- Your hospital stay will be shorter, usually one or two nights compared to 2-4 nights with traditional surgery.
- Recovery is generally faster and less painful.
- This technique causes less blood loss.
Disadvantages of this technique
This technique runs the same risks for incontinence and erectile problems as open surgery.
Laparoscopic prostatectomies have not gained widespread acceptance because they are technically difficult to perform even in the hands of skilled laparoscopic surgeons. Specialized training and equipment are required.
Robot-assisted laparoscopic surgery

In recent years, robotic surgery has developed and become increasingly popular. As the learning curve is faster for robotic surgery than for laparoscopy, this type of surgery is more and more widely used by urological surgeons.
The movements of robotic instruments are intuitive, and the surgeon has a 3D‑view of the prostate. In addition, robotic instruments have articulated tips which mimic human wrist movements.
Advantages of this technique
While this technique generally shortens recovery time, it has not been proven to be any more effective than hand-assisted laparoscopies or open surgeries performed by an experienced surgeon.
- Your hospital stay will be shorter, usually one or two nights compared to 2-4 nights with traditional surgery.
- Recovery is generally faster and less painful.
- This technique causes less blood loss.
Disadvantages of this technique
Unfortunately, patients still run the same risk for incontinence and erectile problems as in open surgery.
There are also economic considerations with robotic surgery—specialized training and equipment are required—and only centres with a high volume of cases can offer this technique.
What is the best technique?
We know that you are faced with a choice between several surgical techniques. Which one is the best? We’re not in a position to say yet. The most important factors are the skill and experience of the surgeon rather than the method used. Therefore, we suggest you talk to your surgeon about his or her experience with the different techniques available. We will discuss this subject a little further on in this page.
Nerve-sparing surgery
Surrounding the prostate are bundles of nerves responsible for erections. When the surgeon removes your prostate, he will try to save these nerves. This is known as “nerve-sparing” surgery.
Whether or not the nerves can be spared depends on how close the cancer is to the nerves. It is difficult for the surgeon to know before surgery if the nerves can be spared. The decision to spare nerves is made once the prostate and the tumour can be seen during surgery.
Success rate
Nerve-sparing surgery is more successful with early stage prostate cancer and for younger, sexually active men.
Advantages and limitations
 Advantages of radical surgery
Advantages of radical surgery
- It removes your cancer completely if it has not spread outside your prostate.
- You will know the exact size and nature of your post-surgery tumour.
- It is easy to measure the success of your surgery by checking your PSA level 6–8 weeks after your operation.
- You have the option of using radiation or hormone therapy if your PSA level rises.
Limitations of radical surgery
- There is always a risk of complications associated with any major surgery.
- You will need to stay in the hospital for 1–4 days or more, if there are complications.
- If the cancer has spread beyond your prostate, the surgeon may not be able to remove it completely.
- You will no longer ejaculate and will not be able to have children after surgery.
Surgical risks and complications
A radical prostatectomy is a major operation, and as with all major operations, there are short-, medium-, and long-term risks and complications. It does not affect all men in the same way—it all depends on the surgery and your general state of health.
Short term
Complications during surgery are rare, but may include:
- Bleeding that may require a blood transfusion
- Damage to the ureter requiring repair
- Rectal trauma or lesions because of its close proximity to the prostate and tumour; usually repaired immediately, with no aftereffects
- Blood clots in the legs that can travel to the lungs
Post-operative
Post-operative complications, once you have returned home, may include:
- Pain
- Nausea and vomiting
- Wound infection
- Urinary infection requiring antibiotics
- Constipation from pain medication
- Bladder contractions caused by irritation of bladder walls from the probe
- Post-operative urinary incontinence and erectile dysfunction in almost all men. Complications are temporary and for many of them things gradually return to normal within a year.
Medium-long term
The most common problems associated with radical prostatectomy are:
- Urinary incontinence
- Erectile dysfunction
- Narrowing of the urethra
To learn more about incontinence or erectile dysfunction, see our section on side effects.
A successful surgery
The success of the surgery and the risk of side effects depend on the experience and skill of your surgeon. Your surgeon should be able to tell you how many operations he has performed, the success rate of these surgeries, and the rate of side effects in his patients.
Surgeons, who are in the operating room on a regular basis (ex. 3 times a month) or perform at least 20 radical prostatectomies a year, ideally more than 35 a year, have better outcomes including a lower rate of side effects.
It is important to note it’s not the number of patients operated on that counts, but the experience of the surgeon. In this regard, ask your surgeon if they can put you in touch with one of their patients. There are also websites where patients give their opinions about doctors. Be careful, as you may become more confused about your surgeon’s skills, as opinions may be completely different from one patient to the next.
If your surgeon has taken the time to talk to you, answer your questions regarding his success rate, his failures, and time spent in the operating room and has given you confidence in his abilities, it is a safe bet that you are in very good hands. And it is definitely the hands of the surgeon that make the difference, regardless of whether the surgery is conventional (open) or robotic.
What to expect
 Your doctor has offered you radical surgery to treat your prostate cancer? This section describes this treatment and the precautions to be taken to ensure that everything goes as smoothly as possible.
Your doctor has offered you radical surgery to treat your prostate cancer? This section describes this treatment and the precautions to be taken to ensure that everything goes as smoothly as possible.
Terminology
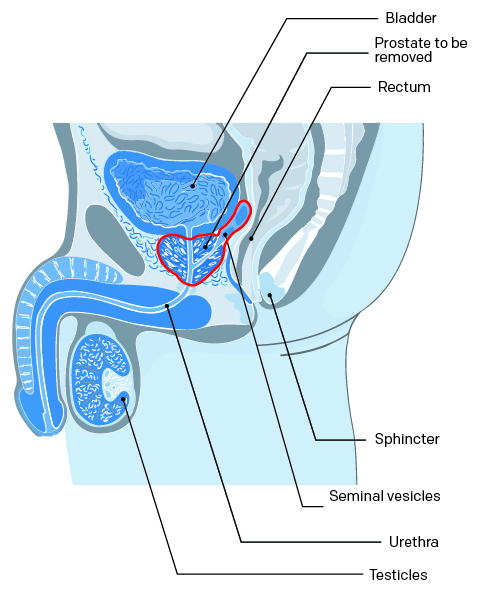
To familiarize you with medical language, here is a brief description of structures that make up the male reproductive system.
Bladder: The muscular sac-like organ in which urine is collected and stored in the body.
Prostate: The gland located just below the bladder that surrounds the urethra. It secretes fluids that mix with sperm cells to form semen.
Rectum: The terminal section of the large intestine.
Sphincter: Small muscle located at the opening between the bladder and the prostate. The sphincter prevents urine from leaking out of the bladder—controlling urinary continence.
Seminal vesicles: Small pouches that store the sperm produced by the prostate.
Urethra: The tube that carries urine from the bladder and sperm secreted by the genital glands out through the penis.
Testicles: The two glands located inside the scrotum that form sperm cells and produce testosterone (male hormone).
The medical intervention
Your hospital stay
You will be hospitalized either on the day of or the day before your operation and will stay for anywhere from 24 hours to a few days, if there are no complications.
Duration of the surgery
Two to 4 hours. If your surgeon tells you that he or she can perform this procedure in less than two hours, get a second opinion.
The operation
You will be given general anesthesia or spinal anesthesia (or an epidural like those given to women in labour) so you won’t feel a thing. During the operation, the surgeon will remove your:
- prostate
- seminal vesicles
- area where the prostate meets the bladder (bladder neck)
- part of the urethra that passes through the prostate
- pelvic lymph nodes
Your urinary catheter
While you are still under anesthesia, a urinary catheter will be inserted through your penis to drain urine from your bladder during your healing process. Your catheter will remain in place for 1–2 weeks after your surgery.
The size and nature of your tumour
In the days following your operation, your prostate, seminal vesicles, and removed tissues will be analyzed by a pathologist. This will allow your surgeon to identify the exact size and nature of your tumour.
Your PSA level
Your PSA level should drop to an undetectable level (0) once your prostate has been removed.
Getting ready
 If you are well-prepared, your post-surgery recovery will be less trying than expected. Being well-prepared will help you recover more quickly and be less stressed. By reading the following, you will know exactly what is waiting for you.
If you are well-prepared, your post-surgery recovery will be less trying than expected. Being well-prepared will help you recover more quickly and be less stressed. By reading the following, you will know exactly what is waiting for you.
Before the surgery
Be active
It is important to move to stay healthy, even if you have prostate cancer. Consequently, if you’re already practicing a regular activity, you should continue doing it until the surgery. If this is not the case, it’s never too late to add exercise to your daily routine; even if it’s at a lower intensity.
Even taking a short 15–30 minute walk can be beneficial.
Do your Kegel exercises
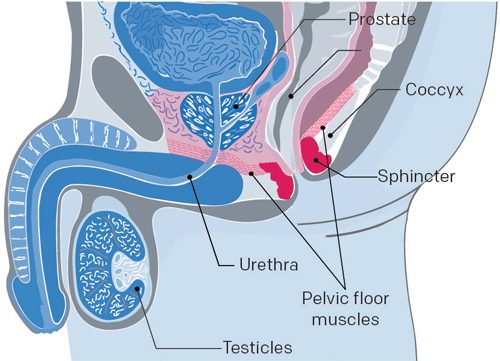
Doing pelvic floor muscle exercises are extremely effective in reducing incontinence after a radical prostatectomy. You should start doing these exercises before your operation and continue doing them after the withdrawal of the catheter. You should see an improvement after 5–6 weeks of regular exercise.
Sit, stand, or lie down with your knees slightly apart—imagine that you’re holding in your urine or bowel movement. Contract the muscles you would use in this situation.
- Contract your muscles for 5–10 seconds.
- Release your muscles for 10 seconds.
- Repeat contractions 12–20 times.
- Do these exercises 3 times a day.
How to know if you’re contracting the right muscles
To know if you’re contracting the right muscles, look at your penis—it should tighten and contract inwards. You should also feel the rectum muscles —the muscles you use to hold in your gas and bowel movements—tighten and contract.
When your muscles are stronger and you are leaking less, you can reduce the exercises to 10 contractions, two or three times a week. Remember that every man is different.
Pelvic physiotherapy
Physiotherapy in perineal rehabilitation is recommended by doctors and aims to strengthen the pelvic floor muscles in order to contribute to a better closure of the urethra. Your physiotherapist, an expert in perineal rehabilitation (important), can advise you on good hydration habits (water resources), constipation control, control techniques for urinary problems and the integration of good perineal contractions at the appropriate times.
Planning your time off with your employer
You won’t have any choice but to tell your employer. Planning your time off and your return to work is important for both your recovery and peace of mind. If you work, you should address the subject as soon as possible. You should be prepared to be away from work.
- Jobs with flexible hours, involving no physical effort: 3–4 weeks
- Jobs involving some physical effort: 6–8 weeks
- Jobs involving excessive physical effort: 12 weeks
After 6 weeks, you may be able to work full-time. The duration of your sick leave will vary depending on the speed of your recovery and the type of work you do.
If you have private insurance, talk to your insurance provider or your company’s human resources department to plan for your absence and minimize your stress.
Try to stop smoking
Even if it’s stressful, it is recommended that you stop smoking 6 weeks before your surgery in order to reduce the risks of lung, healing, and infection problems. If needed, your doctor may prescribe medication to help you.
Reduce your alcohol consumption
Alcohol can also interact with medication. This is why it is recommended to reduce its consumption and not drink in the 24 hours before surgery.
Adopt good eating habits
A healthy and balanced diet will also help you to recover quickly after the surgery. Energy, proteins, vitamins, and minerals that you get from your food can help fight against these infections and help contribute to your healing.
Basic advice for you
- Have 3 meals a day and snacks when you need them.
- Eat food from all four of Canada’s Food Guide (low-fat dairy products, fruits and vegetables, grain products, lean meat, skinless poultry, fish, and other alternatives) in order to ensure you get your daily intake of various nutrients.
- Have at least one meal day that consists of lean meat, skinless poultry, or fish in order to ensure you get your daily intake of various nutrients.
- Fruits and vegetables are an excellent and important source of vitamins and minerals.
- Drink enough water—at least 1 500 mL a day or 6–8 glasses.
Avoid taking medication with acetylsalicylic acid (Aspirin)
If medication is prescribed by your doctor or cardiologist, check with them before you stop taking it. Medication containing acetylsalicylic acid (Aspirin) can increase the risk of bleeding. You will need to stop taking it 7–14 days before the operation.
If you are taking this medication to relieve pain, opt for medication containing acetaminophen (Tylenol).
Avoid natural products
As some natural products can interact with medication given to you at the hospital, it is better to avoid them. If needed, discuss it with your urologist first.
Plan ahead
After surgery, you won’t necessarily have the energy to prepare your meals, complete your daily tasks, or even bathe yourself. If possible, prepare a few meals before the surgery and freeze them. You can then easily reheat them during your recovery.
Ask family and friends to help you with certain tasks if you need it.
Arrange transportation
If there are no complications, you will be able to leave the hospital 1 to 4 days after the operation if everything goes smoothly. However, it could be stressful for you and you won’t be able to drive yourself home. It would be much better if you had someone to take you home. It is also important to note that after your surgery, you should not drive for at least two weeks.
Your preoperative visit
 Before undergoing surgery, you may be required to attend a pre-admission session at your hospital. You will sign a discharge of liability releasing your surgeon and the hospital from any responsibility of risks during surgery. This discharge is mandatory for all surgeries.
Before undergoing surgery, you may be required to attend a pre-admission session at your hospital. You will sign a discharge of liability releasing your surgeon and the hospital from any responsibility of risks during surgery. This discharge is mandatory for all surgeries.
During this visit, you will undergo:
- Blood tests.
- An ECG (electrocardiogram).
- Radiological exams, sometimes.
- A meeting with your anesthesiologist. You will be asked questions regarding your medical history, allergies to medication, and medication you are currently taking. You anesthesiologist will tell you which medication you should continue taking and which ones you should stop taking.
All examinations listed above are done on an outpatient basis a few days or weeks before the operation.
Usually, the meeting with your surgeon has already taken place. If you have other medical problems after your tests, you may be referred to another medical specialist before your surgery.
Admission protocol
The hospital staff will also explain the admission procedure to you and give you any instructions you need to follow before the surgery; such as restrictions on food and beverages after midnight. Find out about the facilities the hospital offers for storing your personal effects.
Your blood donation may be needed
Blood transfusions are rarely necessary, because in general, you will not lose much blood. Nevertheless, as a precaution, some hospitals ask their patients to provide some of their own blood before the operation. This way, if you need a blood transfusion during or after surgery, your own blood will be used. This is known as an “autologous donation”.
It is discarded if it is not used as hospitals are not authorized to keep it or use it for other patients.
Clearing your bowels
You may be required to take a laxative the evening before and use an enema the morning of the operation to ensure that your bowel is clear of fecal matter. One thing is for sure, no food or liquids in the 8 hours before the operation.
The importance of understanding
Side effects related to your surgery
Be sure to have an in-depth discussion with your urologist about the implications of the surgery, the impact it will have on the quality of your life and sexuality, and the tools available that can help you deal with it all. Don’t be afraid of reconsidering or discussing your options again if you are uncertain.
Post-op Prescriptions
It is important to have a clear understanding of the prescriptions your urologist will prescribe for you to take when you get home. Your pharmacists can also give you advice, but you should first talk to your urologist.
Post-op Kegel exercises
Make sure that you also understand how to resume your Kegel exercises.
Post-op penile rehabilitation
Finally, ask about penile rehabilitation and the early use of prescription drugs—erectile dysfunction medications in particular—after surgery to help the penis quickly regain erectile function. Please note that this approach is not universally accepted due to the lack of research on the subject. However, you can discuss the subject with your doctor.
- Usually starts right after your surgery. Low doses are taken daily for several months if you can bear it.
- Some urologists prescribe medication such as tadalafil, sildenafil, or vardenafil immediately—you will find them in your information package when you leave the hospital.
- Other urologists prefer to first discuss it with you at your follow-up appointment.
If your urologist doesn’t bring up the subject during your preoperative visit or follow-up appointment, don’t hesitate to it up yourself.
A few days before
The call from Admitting
The day before your surgery, the Admitting Department will call you to tell you when to arrive at the hospital. You should arrive 2–3 hours before your surgery. The time of your surgery is not final—your surgery could take place before or after the scheduled time.
Cancellations
If you are sick, call your surgeon’s office as soon as possible. If you can’t reach your surgeon, call your hospital’s admitting department.
If your surgeon is late or cancels due to an emergency, your surgeon will postpone your surgery and reschedule it for as soon as possible.
Washing
The evening before the surgery
- Take a shower or bath
- Wash your body from the neck down—don’t forget your bellybutton
- Use regular shampoo and soap for your hair and face
- Wear clean clothes to bed
The morning of the surgery
- Take a shower or bath using the second sponge
- Put on clean clothes
- Don’t put on any lotion, jewellery, or piercings
- Don’t shave the area that is to be operated on
Things you need to bring to the hospital
- Your health insurance card and hospital card
- Any information concerning your private insurance (if you have one)
- Your medication in their original containers
- 1 pack of your favourite chewing gum
- A bathrobe, slippers, and clothing that is loose and comfortable
- Absorbent pads or incontinence underwear (Depends or Tena)
- Your toiletry kit: toothbrush, toothpaste, mouthwash, comb, deodorant, soap, shaving supplies, tissue paper, and earplugs if needed
- Your glasses, contact lenses, hearing aid, and/or dentures with their appropriate storage containers—clearly labelled with your name
- Your cane, crutches, or walker—clearly labelled with your name
- If you’re a techie, bring your headphones and your music
Note
Leave any valuable objects, credit cards, and jewellery at home. The hospital is not responsible for objects that are lost or stolen. Some hospitals will offer you a locker for your personal effects but you may be responsible for bringing your own lock. Find out about facilities your hospital offers for storing your personal effects.
Know that…
You won’t have the time to read because you will be asked to move, eat, drink, urinate, move again, manage your pain, and deal with physical shock. Ideally, if everything goes well, you will be released from the hospital after 24 hours.
During treatment
 The day of the operation
The day of the operation
Make sure you get to the Surgery Pre-Admission office on time
- The admitting attendant will have you sign an admissions form and will ask about your room preference. It is not always possible to get a private or semi-private room.
- The nurse will ask you to put on your hospital gown and will fill in a preoperative checklist with you. You should have been fasting since midnight so your intestines should be empty.
- In some hospitals, you may be asked to wear tight elastic socks to help with blood circulation and prevent blood clots. If this is the case, you should wear them until the nurse tells you to remove them.
The operating room
- An attendant will bring you to the operating room. You will meet your anesthesiologist, the doctor who puts you to sleep, and other members of your surgical team.
- At this stage, there is no point in stressing yourself out or being anxious. You have made the right choice and you are now ready for the next step. Your attitude is vital and will dictate the length of your recovery and facilitate your healing process.
- You will be asleep and feel no pain during surgery.
The waiting room
Your family and friends can wait for you in the room or in the cafeteria. ATMs are usually available in most hospital centres.
During the operation
Your IV
You will be given fluids intravenously until you are able to drink and eat normally. N.B.: When you walk, you will need to push the IV pole with the hand that is not connected to the IV.
Your Jackson-Pratt tube or other post-operative drain
A drain, such as a Jackson-Pratt tube, will be installed in you. The drain is a special tube that prevents blood and fluid from building up inside your abdomen. It consists of two major parts: a flexible tube and a collection bulb. Most patients do not return home with their drain but it is possible. If this is the case, you will be instructed on how to take care of it once you get home.
Your urinary catheter
You will come back from the operating room with a catheter, a tube inserted into your penis called a urinary catheter, which will drain urine from your bladder to a collection bag. You will leave the hospital with your catheter. It is possible for your urine to be tinged with blood—don’t worry.
Your oxygen dose
You might have small tubes in your nostrils to give you oxygen. You will have a small clip on your finger to measure your blood oxygen levels. This is called pulse oximetry. The nurse will adjust the amount of oxygen given to you based on the results and will stop giving you oxygen when you no longer need it.
In the recovery room
 After your surgery, you will wake up in the post-anesthesia care unit, also known as the recovery room. This is a quiet place where patients are carefully monitored. You will stay in recovery for several hours.
After your surgery, you will wake up in the post-anesthesia care unit, also known as the recovery room. This is a quiet place where patients are carefully monitored. You will stay in recovery for several hours.
You will have:
- an oxygen mask, if needed
- an IV line providing liquid
- a urinary catheter (tube) that drains urine from your bladder
- a Jackson-Pratt tube that collects liquid or blood in your abdomen
A nurse will:
- frequently check your pulse and blood pressure
- check your dressings
- make sure that everything is okay
When you are ready, you will be taken to your room. Visitors are not allowed in the recovery room, unless you stay overnight. Your family will be able to visit you when you are in your room.
Pain control
It is normal to feel pain after your surgery. It will feel like a burning or tightening sensation in the area around your incisions. The pain is stronger in the first 24–48 hours and will then gradually decrease.
It is important to control your pain because it will help you to:
- take deep breaths
- move more easily
- eat better
- sleep well
- recover more quickly
- do the things that are important to you
Your nurse may ask you to rate the level of your pain on a scale from 0 to 10. Level 0 means you feel no pain and 10 is the worst pain you can imagine. The staff will want to keep your pain under 4 out of 10. If you are in pain, you need to tell them.
The most common possible side effects of pain medication are:
- Nausea and vomiting
- Drowsiness
- Itching
- Occasional headaches
If you experience any of these symptoms, tell your nurse and they will help you. Remember, it is very important that you not wait until the pain is intense to ask for sedatives. If you do, the medication will be less effective and will delay pain relief.
Exercise and activity
It is important to move around in your bed to avoid pneumonia, blood clots, and loss of muscular strength. Start the following exercises as soon as you wake up and continue doing them for as long as you are in the hospital.
Anti-embolism or intermittent compression stocking
Regardless of the type of stockings, by squeezing the legs a little, blood circulation is improved which prevents blood clots. You may be asked to wear them until you can walk normally. If you don’t have socks, you will be asked to move around quickly.
Move as soon as you wake up
You will be encouraged to change positions and get up frequently. You will slowly progress through the following activities:
- Get up and sit in a chair
- Take short walks around the room
- Take a walk down the corridor at least 3 times a day
Leg exercises
These exercises help blood circulation in your legs. While you are awake, repeat each exercise 4–5 times every half-hour.
- Make circles with your feet to the right and to the left
- Wiggle your toes and bend your feet up and down
- Stretch your legs out horizontally
Deep breathing and coughing exercises
These exercises will help you breathe deeply to avoid lung problems, such as pneumonia. They can be done with or without a spirometer (a device that allows you to see how much air you are breathing and watch your breathing improve). You will be shown how to do them.
For example, without the device, in a sitting or half‑sitting, place a hand on your and the other on your chest, then:
- exhale slowly through your mouth
- inhale through your nose and fill your stomach with air, hold for 3 seconds
- exhale slowly through your mouth
Repeat 8–10 times every hour. These activities help prevent circulatory (phlebitis) and pulmonary (pneumonia) complications. Being active promotes the evacuation of intestinal gas and decreases abdominal bloating.
Goals right after your surgery
In your room the evening of the surgery
- Drink liquids and protein drinks like Ensure and Boost if you can handle it. Your IV will be removed if you drink enough.
- Get up and sit in a chair with or without the nurse’s help.
- Do your breathing exercises.
- Do your leg exercises.
Goals for Day 1
Breathing
- Do your breathing exercises.
Activities
- Eat your meal sitting in a chair.
- Walk down your hallway and try to stay out of bed.
Pain Control
- If your pain surpasses 4 out of 10, tell your nurse.
Eating and Drinking
- Eat regular foods if you can handle it. It is quite possible that you do not have any bowel movements for up to 3–4 days after your surgery.
- Drink liquids. It is important to hydrate regularly by drinking water, juice, tea, herbal tea, or energy drinks like Ensure and Boost—it promotes urinary drainage.
Hygiene
- It is important to keep the area around the opening of your catheter (penis) clean and clear of crust from secretions, at all times. A nurse will help you with your personal hygiene if you need assistance.
Tubes and lines
- For most patients, the Jackson Pratt tube on your abdomen will be removed when you are discharged.
- For some patients, you will keep your drain until your follow-up. appointment. If this is the case, your nurse will teach you how to take care of your Jackson Pratt.
Your Dressing
- Your dressing will cover your wound and the edges of your abdominal drain. It will be changed the day after your surgery. If there is no discharge, the abdominal wound will be left uncovered.
Planning your hospital leave
Your urinary catheter
You will leave the hospital with a catheter in your ureter and a collection bulb attached to your thigh. This apparatus is a little uncomfortable, but it’s invisible under clothing so it won’t be embarrassing. You will also have a drainage bag to use at night.
Before you leave, the nurse will teach you how to take proper care of your catheter and will make an appointment with your CLSC to have it removed at the prescribed time. This procedure is painless and lasts only a few seconds.
Your staples
If you have surgical staples, arrangements will be made with your CLSC to have them removed seven days after your surgery. Butterfly closures can be used to hold the edges of your wound together.
Absorbable sutures
If the surgeon used absorbable sutures—also known as dissolvable stitches—to close the wound, they will disappear on their own after 4–6 weeks. Keep the butterfly closures on for 15 days after the operation.
Your follow-up appointment
You will receive an appointment for a follow-up with one of the members of your urology team about 1 month to 6 weeks after your surgery.
Instructions, care, and hospital contacts
You should receive a document summarizing your care. The document should include instructions for you to follow upon your return home and the telephone contact information of your surgeon and healthcare team should you have any concerns.
Some patients may need an injection of low molecular weight heparin for a month to prevent phlebitis. If this is the case, the procedure will be explained to you.
Before leaving the hospital
You should have a clear understanding of:
- your medication and how to take them
- you exercise program
- your diet
- restrictions
- how to clean your catheter
- how to clean your drain
- what symptoms should call your doctor about
- the time and place of your follow-up appointment
- how to avoid falling down at home
At home
 Your recovery
Your recovery
At home, it is normal to experience:
- Inflammation and discolouration of the skin around the penis and scrotum
- A “burning” sensation where the incision is
- Slight redness along the incision
- Light discharge from the incision
- Fatigue
- Most men experience urinary problems and sexual difficulties at least temporarily
Pain and your medication
- You may have pain for up to several weeks after the surgery. Take acetaminophen (Tylenol) for pain relief.
- If your pain does not decrease with acetaminophen (Tylenol) and anti-inflammatories, add the analgesics that your doctor prescribed.
- If anti-inflammatories or other pain medication causes burning or pain in your stomach, stop taking them and call your surgeon.
- If you have intense pain that cannot be alleviated with medication, call your doctor or go to the emergency department.
- Pain medication may cause constipation.
- To keep your bowel movements regular:
- Drink more liquids.
- Eat whole grains, fruits, and vegetables.
- Exercise regularly (taking a 15-minute walk is a good start).
- Take mild laxatives if it is recommended by your doctor.
Maintain good hygiene
- Only take showers until the incisions have healed (approximately 2 weeks).
- You can shower as soon as your drain is removed and there has been no discharge from your wound in 48 hours.
- Baths, spas, or pools are not allowed for at least 4 months following surgery. Your doctor needs to give you the green light first.
Monitor the healing of your wound
- A CLSC nurse will remove your clips 7–10 days after the surgery. The CLSC will contact you at home. You will then have butterfly closures that will either fall off on their own or will need to be removed 7 days later. You can then wash the wound with mild, unscented soap, rinse it, and pat dry.
- If the surgeon uses absorbable sutures to close the wound, they will dissolve on their own after 4–6 weeks. Keep the butterfly closures on for 15 days after the operation.
- Avoid exposing your wound to sunlight for the first 3 months after your surgery.
Swelling or bruising is normal
- It is normal to have swelling or bruising around your wounds. These reactions disappear with time.
- The scrotum and penis can also become swollen and discoloured. They will gradually regain their normal appearance with time. To reduce swelling, apply an ice pack: while sitting or lying down, place a balled up towel under the scrotum to raise it up to reduce swelling.
Your diet
- There are no restrictions to your diet. You can eat whatever you like. Continue drinking a lot of fluids, at least 8–10 glasses a day, to irrigate your bladder and prevent constipation.
- Eat foods that are natural laxatives like prune juice and dried prunes.
- If that is not enough, an emollient or colon stimulant may be prescribed by your doctor. Do not use enemas.
If you have spasms
- It is normal for you to occasionally experience bladder spasms in the form of contractions around your urethral catheter. You will feel a strong urge to urinate that can come with urine leakage around the catheter’s circumference. Take deep breaths to relax your sphincters. If this happens too often or is very inconvenient, your doctor may prescribe medication to reduce your spasms.
Sexual activity
- You can start having non-strenuous sex at the end of the 3rd week after your surgery. Do not have vigorous sex before the 6th week.
- If you are taking medication to help stimulate an erection, you can take them as prescribed by your surgeon.
Your urinary catheter and collection bags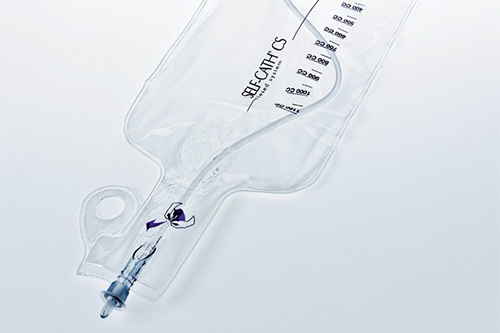
You will have 2 drainage bags and a catheter stabilizer. The catheter stabilizer keeps the urinary tube in place and keeps it hooked to your leg. The small bag is for day and the bigger one is for night.
Use the smaller bag during the day
- Attach the bag to your leg and make sure that it is not too tight.
- Make sure that the bag is low enough so that the catheter won’t get twisted but hangs above the knee.
- Empty the bag every 2 or 3 hours so that it won’t be too full.
- Never let it get more than ¾ full.
Use the larger bag at night
- At bedtime, the bag should always be lower than your body to ensure that urine drains well.
- Empty your urine bag in the toilet every morning.
Penis care and hygiene
- Clean the catheter-meatus area daily with soapy water, then rinse.
- Wrap the penis and urinary catheter with gauze or an absorbent towel to avoid irritating the glans and to collect excess urine that may leak after a bladder spasm.
- Secure the urinary catheter to the abdomen to respect male anatomy and prevent urethral stenosis (narrowing of the urethra).
Before bed
- Decide which side of the bed to install the bag.
- Tape the catheter’s tube to your thigh on the same side as the bag when you’re lying down.
- Leave a little space so that the catheter won’t pull on anything when you move a little at night.
- Once in bed, place the drainage tube so that it can’t bend or form knots.
- Using the hook on the bag, hang the bag on the side of the bedframe.
- Make sure that the bag is always lower than your bladder whether you are sitting, standing, or lying down.
- Do not hang the bag at the head or foot of your bed or off of a chair next to the bed.
What you need to know
- You can take a shower with your catheter and drainage bag, unless told otherwise.
- Keep the collection bag lower than your bladder in order to prevent reflux.
- If there is no urine in the collection bag after several hours, make sure that the drainage tube is not bent or squished.
- Your urine may be cloudy in the beginning, but will be back to normal after a few weeks.
- It is normal to have blood in the urine after this surgery. If you see blood in your urine, drink more and decrease your activity until your urine clears up. If you have done this and still see no change, call your surgeon’s office.
- Always make sure that urine continues to drain into your bag.
- If the catheter slips out, go to the Emergency room.
Care of your catheter and bags
How to switch from one bag to the other
- Empty the urine from your bag into the toilet.
- Wash your hands.
- Disconnect the new bag and clean the cap with rubbing alcohol for 15–30 seconds, then place the bag on a clean towel.
- Clean the connection between the urinary tube and your urine bag with a new alcohol swab for 15–30 seconds before disconnecting it.
- Disconnect the urinary tube from the urinary bag.
- Reconnect the urinary tube to the new urinary bag.
- Protect the end of the tube not being used with a sterile protective cap.
- Close the clamp and attach the belt around your thigh.
- Wash your hands.
Always
- Keep the caps from the bags.
- Keep the caps clean.
- Cover the caps when not in use.
- Keep a cap over the tip of the unused bag.
How to clean your bags
- Wash your hands and disconnect the bag.
- Empty the bag and rinse with tap water (use a small funnel or plastic cup).
- Fill the bag with a vinegar solution.
- Gently shake the bag filled with the vinegar solution and let it hang for 30 minutes.
- Empty the bag and air dry.
- Store in a clean dry place.
- Wash your hands.
Note
You should clean your bags every day. You can use the 2 drainage bags for a maximum of 1 month. You must then buy new ones. They are available in most medical supply stores.
After Removing your Catheter
Resume your Kegel exercises and develop good habits to manage urinary incontinence:
- Do not get into the habit of going to the bathroom “in case” and only go when you really need to. The standard is 3–4 hours a day and just before going to bed.
- Empty your bladder regularly.
- Sitting when you pee helps to empty your bladder.
- Learn to tighten your muscles before you sneeze, cough, laugh, or get up from a chair.
- Avoid over-consumption of alcohol, coffee, soft drinks, chocolate, and aspartame that are bladder stimulants.
- To avoid excessive stretching of the pelvic floor, do not push too hard during a bowel movement. Start eating a high-fibre diet to prevent constipation.
- Insert the smallest protection pad possible into your pants.
- While training your bladder, use a bladder diary so that you can identify bad habits and regulate your urinary continence cycle.
Care of your Jackson-Pratt tube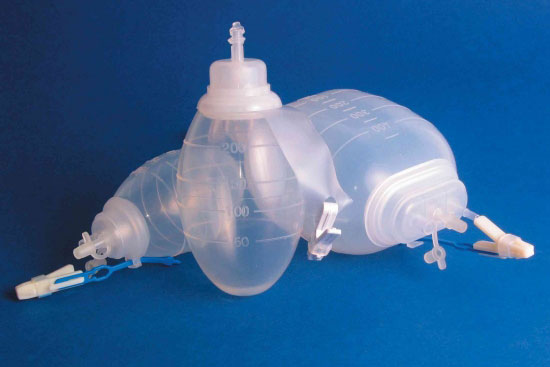
The Jackson-Pratt tube is connected to a bulb-shaped container that looks like a grenade. This container collects the fluid that drains from the incision and helps healing.
At first, the liquid might be tinged with blood. After a few days, there will be less fluid and it will become a clear yellow.
How to empty your tube
- Wash your hands before touching the Jackson-Pratt.
- Open the cap. The bulb will take back its shape. The Jackson-Pratt bulb is like a measuring cup.
- Record the amount found in the bulb in your bladder diary.
- Squeeze the bulb to empty the fluid in the bulb into the toilet.
- Close the cap while squeezing the bulb.
- Let go of the bulb. It will slowly fill with liquid again.
Activities
Resuming activities at home
- Continue to take walks several times a day. Progressively increase the distance you walk until you are back at your normal activity level. Most patients do not have many exercise restrictions.
- Do not drive while taking analgesics.
- Your surgeon will decide when you can return to work. This will depend on your recovery and the type of work you do.
- You will probably return to work a few weeks after your surgery on the condition that you do not lift any heavy objects.
- Wait 6 weeks before doing any demanding sports or abrupt movements (e.g., tennis, badminton, jogging, and downhill skiing) and when you do, do it gradually.
- If you are a cycling enthusiast and your surgery has gone well, there are no post-operative complications, and you recover your continence well, you could be back in the saddle 8 to 12 weeks after the operation. It is always best to ask your doctor for the green light.
Ask your family and friends for help with
- Moving around
- Preparing meals
- Washing
- Grocery shopping
- Cleaning
Bathing
- Not for at least 4 weeks. Wait until the staples and butterfly closures, Jackson-Pratt, and/or dissolvable stitches, stop leaking discharge from the wound, if necessary.
Travelling
- Local and regional: On discharge from the hospital, provided that you make frequent stops every hour.
- International: Avoid destinations where medical services are not readily available (discuss it with your doctor).
When should you call your doctor
Wound infection
(Inform your surgeon and local CLSC)
- Redness
- Heat
- Discharge
- Swelling
- Pain
- Chills and fever (higher than 38.5 oC or 101.3 oF), go the the Emergency room.
Urinary infection
(Inform your surgeon and local CLSC)
- Burning sensation when urinating
- Persistent feeling of not having emptied the bladder
- Heaviness and discomfort above the pubis
- Frequent urination and urinary urgency
- Chills and fever (higher than 38.5 oC or 101.3 oF), go the the Emergency room.
Narrowing of the urethra or bladder neck
(Inform your surgeon or the urologist on duty)
- Difficulty urinating
- Feeling of not having emptied the bladder
- Decrease in the size of your urine stream
Thrombophlebitis
(Go to the Emergency room and inform your surgeon or the urologist on duty)
- Pain and tenderness in the calf that increases when walking
- Local redness
Pulmonary embolism
(Go to the Emergency room without delay)
- Sudden onset of chest pain similar to angina
- Difficulty breathing
- Fever
- Rapid pulse
- Coughing
- Sweating
Infections (various)
(Go to the Emergency room and inform your local CLSC)
- Fever (higher than 38.5 oC or 101.3 oF) on consecutive instances with an interval of 4 hours between each instance.
- Nausea, vomiting, diarrhea, and bloating
If your catheter falls out
(Go to the Emergency room without delay)
- Do not reinsert the catheter. go to the emergency room
- Do not let anyone take out your catheter without your surgeon’s permission
If you are worried that you’re feeling worse with each hour that passes:
- Contact INFO-SANTÉ at 811
- In case of emergency, contact 911
- If you cannot contact your surgeon, go to the Emergency room
Medical follow-up
 The importance of follow-ups
The importance of follow-ups
Medical Certificate
If you need a medical certificate, don’t forget to ask your surgeon directly at least the day before your hospital stay.
Follow-Up
You should see your urologist 4–6 weeks after you are discharged from the hospital. After this first appointment, you will see your urologist at regular intervals (3–6 months). If everything goes well, after 5 years in remission, follow-ups will become annual.
Results
It is impossible to estimate the average success rate of radical surgery.
PSA test
Your urologist will do a PSA test every time since this test is the best predictor for the risk of recurrence of prostate cancer. A digital rectal exam may also be performed sometimes.
PSA level
After the operation, the PSA level should be undetectable (0) since there is no more prostate to produce antigens. At each medical appointment, your urologist will check 3 parameters:
- if the PSA level is higher
- how much time has it been since the operation and
- how much time does it take this level to double (velocity)
Recurrence
If the PSA level starts to climb, the doctor will monitor how much time it takes to double. The shorter these periods are, the greater the risk of recurrence and the more aggressive the recurrence will be. For example, the PSA level that starts to increase eight months after the operation and that doubles in six months is much more worrisome than a PSA level that starts to climb three years after surgery and takes a year to double.
If necessary, radiation therapy and/or hormone therapy may be prescribed.
Remission
After five years without recurrence, you are considered to be in remission and the risk of recurrence is very low.
Side effects
 The most common problems associated with radical prostatectomies are urinary incontinence, erectile dysfunction, and stenosis (narrowing) of the bladder neck.
The most common problems associated with radical prostatectomies are urinary incontinence, erectile dysfunction, and stenosis (narrowing) of the bladder neck.
Urinary incontinence
After the surgery, practically every man experiences a transitory period of urinary incontinence. This period can last for several weeks up to a few months (average 3 to 6 months). For some men, patience will be required, since recovery may take longer (6 to 9 months) and even up to 2 years. It varies from one person to the next depending on the degree of their disease, their age, and their state of health. In most cases, urinary incontinence disappears with time and with specific exercises such as Kegels.
In a few cases, urinary incontinence can be permanent and may require a surgical implant if you are a good candidate for it.
Narrowing of the bladder neck
The suture between the bladder and urethra can scar, causing a fibrosis and a narrowing of the urethra, in less than 5% of cases. This can make urinating difficult (weak urine stream and incontinence) and, in some cases, painful. This problem can easily be corrected naturally with dilation (widening).
Erectile Dysfunction (ED)
A certain percentage of men regain erectile function 6–36 months after surgery. The speed with which their sexual function improves depends on sexual function before the operation, age, general state of health, and preservation of erectile nerves during surgery.
In some men, the surgeon is unable to save the nerves and there is a possibility of the erectile dysfunction persisting without treatment.
Treatments
Treatments include oral medication such as tadalafil, sildenafil, and vardenafil; the MUSE pellet; penile injections; vacuum pumps; or surgical penile implants.
Penile rehabilitation
It is recommended that you do not remain sexually inactive. Penile rehabilitation, to ensure that your penis has a satisfactory erection, is extremely important after surgery. The best thing to do is to discuss it with your urologist before your surgery.
Your ejaculations
After this type of operation, you will no longer have an ejaculation; the seminal vesicles and prostate that produce seminal fluid (semen) have been removed. This is what we call a dry orgasm. The absence of sperm will result in infertility.
Your libido and orgasms
Your libido and orgasms will still be there. There may be a small amount of urine that leaks out during intercourse because the sphincters relax. This is why it is better to urinate before having sex.
Penis shortening
Some men find that radical surgery shortens their penis. It seems that this is not really the case. This impression may come from the fact that when you go a long time without having an erection, the penis can retract from lack of blood flow.
To avoid fibrosis—the hardening of penile tissues caused by the lack of blood and oxygen—men are encouraged to have erections, with or without treatment, as soon after surgery as possible. This will speed up the recovery process and your ability to have an erection while reducing the risk of your penis shortening.
To learn more about incontinence or erectile dysfunction, take a look at our section on side effects.
Suggestions and advice
 Give yourself time
Give yourself time
- There is a lot of information to retain. Don’t try to learn it all in one day.
- You will have questions. Write them down and bring them with you to your next appointment.
- Your body needs time to recover after the surgery.
A healthy lifestyle will help you feel better
- Eat healthy
- Sleep a lot
- Do activities that you enjoy and that relax you
- Socialize
Accept help from others, they want what is best for you
- Practical help
- Emotional support
- Delegate tasks if you need to
- Do not be embarrassed to ask for help
Spend time with others and give them your attention
- Your friends and family also need comfort
- Keep a good line of communication open
- Resolve problems when they happen
Your intimacy
After a radical prostatectomy, many men have mood swings and feelings of sadness, happiness, and fear.
They also stressed the need to continue having intimate relations with their partner despite their inability to have full intercourse. Touching, kissing, holding hands, walking together, talking at length, and just being together can be deeply satisfying and help you recover.
Orgasms will return in due time. We recommend that you talk openly with your partner about your thoughts and concerns and with your urologist.
Maintaining a fulfilling sex life
Things to remember when you are ready to resume sexual activities
- It recommended that you wait 4 weeks before having sex.
- Be prepared for the unexpected and laugh when it happens. Sex is not a “serious affair” or a “marathon”. Stop and rest if you are tired.
- Sex should not cause any discomfort or pain. If this happens, talk to your doctor or nurse. Fear of pain can cause sexual difficulties.
- Performance anxiety can occur if you are too focused on your erection.
- The skin is the largest sexual organ and the brain is the largest sexual organ. Using both allows for endless possibilities when it comes to sex.
- A cancer diagnosis or its treatment should not control what a man can or cannot do. Use your imagination and humour to explore new ways of staying intimate.
Questions to my doctor
Here are some questions you can ask members of the health care team about surgery. It may be useful to bring this list to your next doctor’s appointment to write the answers.
Read more…
- What options are available to remove cancer? What surgery do you recommend?
- What are the benefits and risks of surgery?
- How is surgery performed?
- Will lymph nodes be removed during this surgery? If yes, why?
- What type of anesthesia will be administered?
- Will a blood transfusion be required during surgery?
- How long will the surgery last?
- Is there a waiting list for surgery?
- What are the chances of treatment being effective? When will we know?
- Is a preparation necessary before surgery?
- What tests are done before surgery?
- What are the possible side effects of this operation? When could they appear? In general, how long do they last?
- What side effects should I report immediately? Who should I call?
- What can be done to relieve side effects?
- How will pain be relieved after surgery?
- Will nursing be needed at home? What services to the community can be useful after surgery?
- Will a special diet be required?
- Are there particular things to do or not to do?
- Will this surgery affect normal activities? If so, for how long?
- How long does it take to get the results after the surgery?
- Who will explain the results after surgery?
- Will other treatments be needed after surgery? If so, what type?
- How often are follow-up visits scheduled? Who is responsible for follow-up after surgery?
We are here for you
You have questions or concerns? Don’t hesitate. Contact us at 1-855-899-2873 to discuss with one of our nurses specialized in uro-oncology. They are there to listen, support and answer your questions, and those of your family or your loved ones. It’s simple and free, like all of our other services.
Also take the time to visit each of our pages on this website, as well as our YouTube channel, in order to get familiar with the disease, our expert lectures, our section on available resources, the support that is offered to you, our events and ways to get involved to advance the cause.
Staying Informed
Pages that might interest you
Want to know more? Just click on one of the links below.
The latest PROCURE news that might interest you
Every week we publish a blog article. Here are some we have chosen for you.
- Did you say prostate cancer?
- I want to postpone my treatment… Is that wise?
- I have several treatment options… Which one to choose?
The medical content and editorial team at PROCURE
Our team is composed of urologists, and nurses certified in uro-oncology with a deep knowledge of prostate cancer and other diseases related to the genitourinary system. Meet our staff by clicking here.
Sources and references
- Prostate Cancer – Understand the disease and its treatments; Fred Saad, MD, FRCSC and Michael McCormack, MD, FRCSC, 4th et 5th editions
- Canadian Cancer Society
- Prostate Cancer Foundation-PCF.org
- National Cancer Institute-USA
- American Cancer Society
- Memorial Sloan Kettering Cancer Center
- Prostate Cancer UK
Last medical and editorial review: September 2023
Written by PROCURE. © All rights reserved




